Your Medical Plans Compared
In-network vs. Out-of-network
Both the PPO and the HDHP will have the same network of doctors that are considered in-network versus out-of-network. Staying in-network for all services, providers, and facilities is imperative for you and your family to receive the richest benefit from your medical coverage. The out-of-network coverage is based on the allowable amount applicable for the same service that would be rendered by a network provider and you may be balance billed for anything over this amount.
Preventive Care
You will see both plans also cover preventive care at 100% on the first day of your plan before satisfying your deductible. Examples of preventive care are:
- Well-child visits
- Annual checkups
- Age and gender-based screenings
Finding a Provider
To find a UnitedHealthcare Provider, visit UHC.com
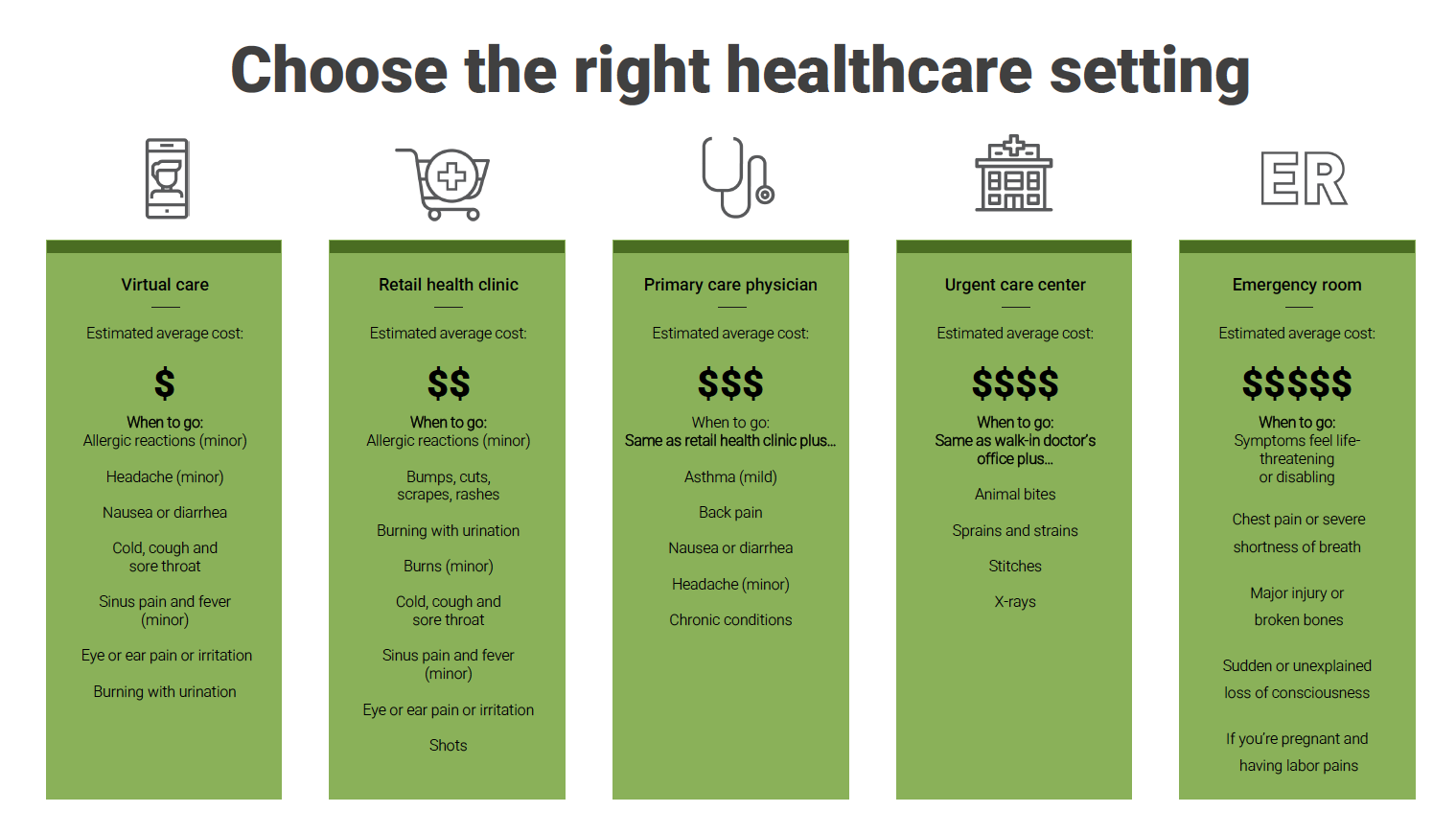
Where to Seek Care
It can sometimes be difficult deciding where to seek medical help for you and your family members. Going to the emergency room or calling 9-1-1 is always the best option when it’s an emergency. If you need care, and it is not an emergency, here are alternative options:
- Call your doctor
- Visit a retail health clinic
- Head to an urgent care facility
- Check-in at Virtual Visits online
Differences
How Your Benefits Pay on PPO
If you are currently on the PPO plan, this option has more coverage from day one of the plan. This is called first dollar health coverage. You will have copays for different services as well as prescriptions before meeting your deductible, which apply directly to your out-of-pocket maximum. You will pay these copays and coinsurance until your medical and prescription out-of-pocket maximums are met.
How Your Benefits Pay on HDHP
The High Deductible Health Plan will not have copays on the first day of the plan. You will start by paying the negotiated rate your carrier has with your providers for any services and prescriptions. You will pay this negotiated rate until you satisfy your deductible and out-of-pocket maximum. After this amount is satisfied, all services and prescriptions will be covered in full.
Surcharges
Health Screening Surcharge
You must have a preventive screening completed or you will be subject to pay a $50 monthly surcharge. Forms must be completed and submitted to the Treasurer’s Office no later than December 1st prior to the beginning of the plan year.
Spousal Surcharge
If you carry your spouse on Montgomery County ESC’s plan and they have access to other group health insurance through their employer, they will need to join their employer’s health insurance and terminate Montgomery County ESC’s or you will be subject to a $100 monthly surcharge.